Background: Robotic Process Automation (RPA)
- RPA technologies function by mimicking human decision making process during the processing of a transactional event in the customer application ecosystem.
- A variety of organizations have mushroomed and are building scale promoting applications that “record and play” or “configure” the software programs or “robots” so either whole transactions or a part of the transactions in customer environment are performed in place of a human agent.
- A Command Center helps monitor the performance and progress of a worker robot such as productivity per hour while checker robots can help evaluate quality of work performed by the worker robot.
- All business rules are codified in centrally hosted libraries and are accessed and used by the configured robots to perform the work activities. Ongoing maintenance of the business rules ensures that they are kept up-to-date and that the work activities are accurate.
- Extended testing is done to ensure required level of accuracy and dependability before letting robots go-live! A smart command center monitors the performance of the robots and makes decisions on starting or suspending the robots.
- Effective governance, self-learning, and an analytics engine open the future of RPA to a path of intelligence decision making through Machine Learning and Artificial Intelligence.
RPA Market Experiences in RCM

- Application of RPA technologies and processes in the healthcare RCM arena have been around for a few years now with varying degrees of success. Despite all the hoopla around automation and varied claims of success, it is safe to say that there is enough hype around the claims of scalability, configurability, and worker displacement. These limitations can be broadly attributed to the challenges in the following three categories: process variability; limitations and lack of openness among EHR application vendors; and slow evolution and expensive nature of automation technologies.
- Healthcare RCM processes comprise various activities such as eligibility verification, authorization, charge capture, coding, claim scrub, payment posting, and AR and denial management. These processes accommodate various nuances, such as specialty, regulations and guidelines from bodies such as CMS or TMHP etc. Given the same, the data required for these processes is spread across multiple sources and other applications and therein lies the complexity and challenge of automation.
- The application ecosystem around which automation has to be implemented typically comprises a workflow platform (or a Business Process Management software) where billing activities are tracked, EHR systems where medical record data is accessed, coding applications where medical coding is performed, a billing platform where actual billing is carried out, insurance web portals where key information is made available regarding a patient’s coverage or the status of a claim, and many other such applications. The multitude of these applications and the challenges in both getting access to these applications for an automation BOT program and recalibrating the BOT program continuously as these varied applications go through refresh cycles has the potential to reduce the efficiency and effectiveness of automation. However, if the EHR and billing software vendor enables data transfer through HL7 protocols, that can simplify the challenge of depending on third party automation platforms and bring into play several point solutions that are developed and already available in the market.
- Vast majority of automation technologies and platforms in the market rely on “record and repeat” philosophy. This requires one to create a standard template by recording the complete screen by screen process flow including the applicable business rule logic in its business library before the template could be used to process similar transactions. Given the process variability discussed above, this process leads to defining several templates which in turn increase the development and maintenance effort. In addition, factoring in the license fees that need to be paid for using these technologies, the automation proposition becomes expensive. Finally, if one considers the difficulty of hiring and retaining qualified and certified automation engineers, the development and deployment lifecycles and costs become unpredictable and the overall ROI a challenge.
RCM functions – Feasibility & ROI: AllySmartRPA Ready Reckoner
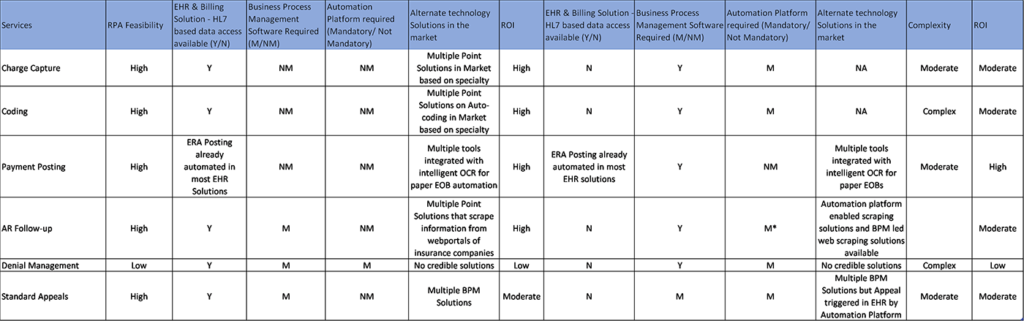
Note:
- M/NM: Mandatory or Non-Mandatory
- Please note there have been several broad-level assumptions made in producing the simplified picture above and as such may or may not be exactly applicable to your operation on account of several, already stated co-dependencies.
In conclusion, a review of the above table shows that it will be advantageous to work with EHR vendors and gain greater control of the data to achieve higher ROI. This will reduce the need for an automation platform and instead one can consider using other less expensive point solutions in the market and achieve higher operational efficiencies. However, the point solutions in the market are dependent on the type of specialty and can impose limitations on what is feasible. Besides, there can be additional constraints based on the effectiveness of the BPM workflow solution. Limitations on these fronts drive the need to utilize a suitable automation platform to derive ROI.

